Sign Up for Our
Updates
I was struck last week when I heard a BBC News reporter on TV use the words “shell shocked” to describe NHS staff battling against Covid in our hospitals.
Thoughts were conjured up of the First World War and the unrelenting horrors endured by the young men who lived through it.
It occurred to me that 100 years ago the roaring 20's must have roared quite differently for some, as by then, after the First World War had ended, the impact of extreme trauma experienced by some men who fought on the frontlines in Europe was having a lingering effect. This was both in the minds of the soldiers who had returned and in society, which had realised something wasn't right with a lot of the young men who had been exposed to the worst of the war.
Some of the soldiers who had returned home to their families were experiencing psychological and physiological effects that were ever-present and debilitating. The condition came to be known as shell-shocked. Many decades later, following the war in Vietnam, lasting symptoms of mental trauma were diagnosed as Posttraumatic Stress Disorder (PTSD) when the American Psychiatric Association added PTSD to its Diagnostic and Statistical Manual of Mental Disorders classification scheme.
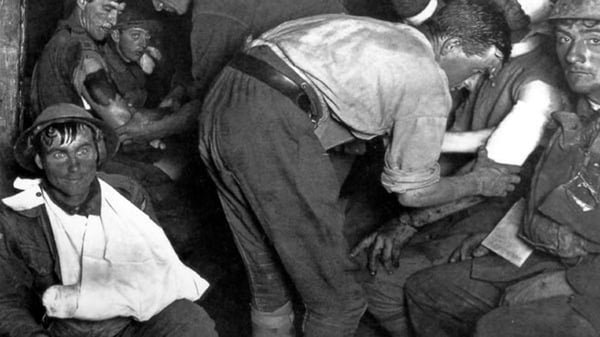
Healthcare might not have yet reached the darkest depths and scale of this trauma, which was experienced in the trenches of the “great” war or the jungles of Vietnam, but comparisons are right to be drawn.
The cognitive strain from persistent, high-attention workload and being in frequent close quarters to human death and suffering is a potent mix of burnout and psychological trauma.
Of course, the trauma of war is different in that it exists not only in the horrors inflicted by the enemy, but also upon them. This exacerbates psychological problems and is a distinguishing factor between shell-shock and "covid-shock", where the battle being fought is to extend life, not take it away. This might hopefully mean diagnoses of more severe PTSD for health workers will be less common than after extreme warfare.
One thing that is certain is that conditions are severe for hospital workers right now. The situation is highly concerning and requires very careful handling and planning. Employee welfare in the immediate and longer term needs to be a central consideration in any wider reform that is surely imminent in healthcare.
Steps will be taken, by those in the correct positions of responsibility across the NHS, to underwrite the wellbeing of those frontline staff affected. However, a considered and planned response is needed to create an environment that is properly geared towards the welfare of the workforce. Tangible, on-the-ground solutions to care for frontline health workers are needed long after the gruelling Covid battle shifts are over. This HR form of care is paramount and cannot be in any way restricted by a lack of financial and structural support from government.
Solutions for "Covid-Shock"
Relief is needed the form of additional staff resources and efficiency-based solutions that reduce burden on shift workers. Focus needs to be on both reducing hours and making work more efficient and easy, however, in an industry that's long suffered significant staff shortages, the former is not straight forward.

Minister of State for Care, Helen Whately, announced this week £7.5 million in funding for the NHS to roll out more e-rostering solutions. 38 more Trusts will, as a result, benefit from being able to digitally match staff skillset with patient care requirements and geography whilst also bringing efficiency into pay and shift management.
This is welcome from NHS England/Improvement and NHSX. It forms part of a wider commitment to deploy technology that helps maximise staffing efficiency.
This couldn't come soon enough.
Another welcome embrace of improved efficiency is the increasing awareness across the NHS through 2020 that process automation, User Experience (UX) and better interoperability across systems has the effect of lessening workload on staff. Much, however, needs to be done to better educate within the NHS in these areas. An example of this is in Process Automation, which remains poorly understood in healthcare and incorrectly synonymised with Robotic Process Optimisation (RPA), a method of process automation that relies on the Graphical User Interface (GUI). RPA has some usefulness, but when procured as a result of being hyped up, it leads to inefficiency and a lack of robust transformation.
Technology, however, is not a substitute for practical human policy. Technology-based solutions are welcomed to help relieve staff burnout and can play a key role in derisking mental health issues, but support is also needed through direct investment in policies that will ensure affected staff are given ample opportunity and encouragement to take as much time off as is deemed necessary to maintain wellbeing, now and long into the future. The ability to do this requires the bolstering of staffing levels. Technology can help with efficiency on the job and in staff management, but alongside this more trained people are needed in the system.

A philosophical revolution
Improving staffing in the NHS requires people to be attracted to it from other industries and more effective recruitment of students.
"I'm not sure if there is anything less cool to a hip 21 year old in the 2020's than a Rolex and a Private Jet"
I'm reminded frequently that we are in a "fourth industrial revolution", which is changing how we work due to technological advancements. This may well be the case, but what gets talked about far less in all our focus on technology, is the gradual but sweeping change in the way younger people now view work, careers, purpose or even that most complicated of words, happiness.
When I speak to people from the so-called "Z" generation, it's things like positive impact and helping the environment that truly motivates them, not wealth. I'm not sure if there is anything less cool to a hip 21 year old in the 2020's than a Rolex and a Private Jet. Current Governments need to recalibrate and harness this more effectively. Nowhere will this bring about more immediate and useful change than in healthcare presently.
The pandemic has obliterated whole swathes of the workforce; some temporarily, some indefinitely. This brings forward an abundance of people who are able to retrain into the human services sector and healthcare. For some time now, there has also been a growing aspiration from the younger generation to choose a career that puts purpose ahead of personal wealth and I have maintained for a long time that healthcare, in particular, the NHS needs to better channel this. In the case of nursing, the issue is the level of salaries, which are known to be low compared to the level of work needed. There is also a perception issue, as was well articulated in the Oxford Brookes study in 2019, which explains that the exciting, cutting edge, innovative and technical side of nursing is not relayed in recruitment campaigns. Improvements in pay would not only directly impact people's financial comfort, but it will also help reflect nursing in a more aspirational light than it currently is. I'm reminded of the recruitment campaigns from the Royal Navy and the British Army. They speak to the youth far better than nursing recruitment does, for example. This is where a recalibration is needed.
The Princes Trust charity in the UK does some great work to train younger people into areas like nursing, but this is relying on Non-Profits where Government should be doing more directly. Most nurses or people choosing careers in areas such as Science, Technology, Engineering, and Mathematics (STEM) are not seeking top-end salaries, but a comfortable wage. Society need only make manageable adjustments to successfully shift towards better recognition of the importance of this type of work and better balance pay with a job's worth in, and value to, society.
Better incentivising work in areas such as life sciences, technology, environment, healthcare and education not only brings immediate practical benefit by solving staff and skills shortages, such as exists in healthcare and technology, but it ultimately contributes to a more equitable, innovative and progressive world for us to all live in. Savvy politicians should (and will) increasingly channel this, tapping into the zeitgeist, and turn attention and policies to sectors such as human services instead of Finance etc. which has traditionally benefitted from being cosied up to.
Whilst societal changes are needed on a macro level and I do believe we are on the cusp of seeing a significant redistribution of wealth towards human services and life science industries, action is nevertheless needed now to support frontline health workers.
As increased staff resources do begin to be available, any time taken off by frontline NHS staff at risk from trauma or burnout from fighting COVID, whether holiday or any leave type, must not translate to any income being deprived to that individual.
Much of the technology sector has for a while now offered perks like unlimited holidays as it has recognised that better work-life balance builds better, more successful companies and happier society. Healthcare and the public sector, through remodelling, can and should mature its thinking and do the same.
I would take this one step further. Incentives that might encourage a health worker to increase hours in order to earn more money should be carefully, but totally, removed by HR teams across the NHS. The temptation to earn more for a nurse, porter or junior doctor on a low/modest salary will otherwise result in more work being done by individuals that need protecting from burnout or worst still PTSD, which should that happen would ultimately cost the public purse more anyway.
Higher, comfortable salaries that are fixed and not in any way linked to hours worked must be brought in to support the health and wellbeing of NHS workers.
There is clear evidence of the debilitating effects from mental trauma resulting from sustained periods of exposure to death and suffering. This is not limited to humans either. During the mass cullings of the foot and mouth crisis in the UK, many workers suffered from mental health problems. Whilst NHS staff are not killing-to-order, being around increased levels of death coupled with the sheer strain of trying to keep people alive is, without doubt, putting their mental health at risk.
The stark reality being that in just doing their job, health workers are having to muster up every bit of inner strength to keep people alive. These are people who have come into their lives as strangers, but who they bond with as humans and, when all they've done to save them fails, hold hands with as they die.
This is happening right now on the wards of our hospitals, and indeed some care homes, and it's intimacy and strain is harming the wellbeing of staff. Everything that can be done to help these brave health workers, must be done.
"Improvements in economically developed countries towards mental health awareness in recent years might just have come in the nick of time..."
Thankfully, since 1918, increased awareness of mental health and PTSD means societal neglect or ignorance towards people at risk should not be the problem it was some 100 years ago. However, PTSD remains, despite its classification, quite poorly understood, but recognition exists that support is needed. This can come through clinically prescribing talking therapies, such as Cognitive Behavioural Therapy (CBT) or broadly and simply there being better care and support for affected individuals and their families.
Improvements, at least in economically developed countries, towards awareness of mental health in recent years might just have come in the nick of time, but financial support and societal compassion must also be invested in to ensure appropriate protection of health workers through the difficult months and, sadly for some, years to come.
Knowing that many of these workers are nurses and that they have been continually undervalued for decades rubs salt in the wound. Thankfully, it feels like this has hammered home the pay issues in the nursing profession. Tipping point or turning point, questions are rightfully being asked. Why, as a supposedly developed society, do we not distribute societal wealth more towards the nursing profession and away from a greedy finance sector that's evolved into an ugly beast? One that at its most worst is parasitic.
Some may read this blog and take the view that the points I am putting forward are idealistic or simply a nice notion without means of being budgeted for. If this is you, I put it to you that this is no fanciful dream. Right now the world needs, and has for some time, innovation and efficiency in sciences, human services, health and data sciences and in industries like logistics. By leveraging existing strong foundations in these sectors and by investing further, countries like the UK can tilt economies to better support healthcare whilst simultaneously growing expertise and fostering innovation in areas like AI, health data, science and genetics, which in turn will drive inward investment as globalisation presses on.
Better mechanisms to redistribute wealth that's already in the system are also much in need. Plenty of money is jangling in pockets of the economy and, in many cases, continuing to be made in areas like banking. The issue is it's being hoarded.
Cunning Traders in the now-virtual-City have profited in big ways by short-selling this downturn. As they've traded and amassed personal wealth, underpaid nurses have commuted into work every day and fought to keep people alive. Exhausted, and in some cases traumatised, they've risked their lives and health whilst earning not much more than the minimum wage.
Enough is surely enough? I'm calling time on a broken system.
By investing properly now in staffing shortages and solutions that improve system-level efficiency and the wellbeing of health workers, society can, and I believe will, evolve and rebalance. In the UK and many other countries, this must not be a symbolic gesture, but be an part of a lasting, system-wide remodelling of the economics of healthcare.

.jpg)
.jpg)